To understand COPD, it helps to understand how the lungs work. The air that you breathe goes down your windpipe into tubes in your lungs called bronchial tubes or airways.
Within the lungs, your bronchial tubes branch into thousands of smaller, thinner tubes called bronchioles. These tubes end in bunches of tiny round air sacs called alveoli (al-VEE-uhl-eye).
Small blood vessels called capillaries run through the walls of the air sacs. When air reaches the air sacs, the oxygen in the air passes through the air sac walls into the blood in the capillaries. At the same time, carbon dioxide (a waste gas) moves from the capillaries into the air sacs. This process is called gas exchange.
The airways and air sacs are elastic (stretchy). When you breathe in, each air sac fills up with air like a small balloon. When you breathe out, the air sacs deflate and the air goes out.
In COPD, less air flows in and out of the airways because of one or more of the following:

The airways and air sacs lose their elastic quality.

The walls between many of the air sacs are destroyed.

The walls of the airways become thick and inflamed.

The airways make more mucus than usual, which tends to clog them.
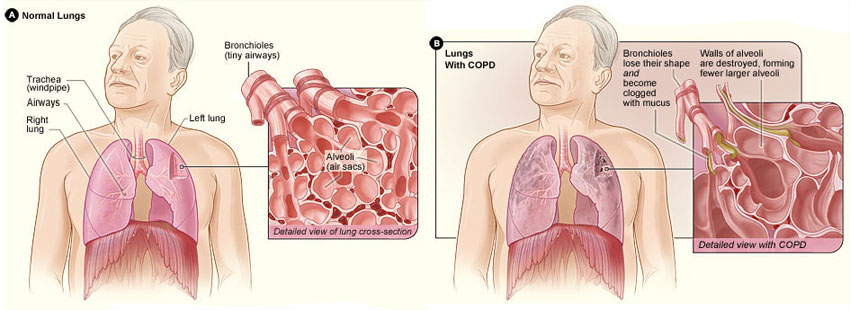
Figure A shows the location of the lungs and airways in the body. The inset image shows a detailed cross-section of the bronchioles and alveoli. Figure B shows lungs damaged by COPD. The inset image shows a detailed cross-section of the damaged bronchioles and alveolar walls.
In the United States, the term "COPD" includes two main conditions—emphysema (em-fi-SE-ma) and chronic bronchitis bron-KI-tis).
In emphysema, the walls between many of the air sacs are damaged, causing them to lose their shape and become floppy. This damage also can destroy the walls of the air sacs, leading to fewer and larger air sacs instead of many tiny ones. If this happens, the amount of gas exchange in the lungs is reduced.
In chronic bronchitis, the lining of the airways is constantly irritated and inflamed. This causes the lining to thicken. Lots of thick mucus forms in the airways, making it hard to breathe.
Most people who have COPD have both emphysema and chronic obstructive bronchitis. Thus, the general term "COPD" is more accurate.

COPD, or chronic obstructive pulmonary disease, is a progressive disease that makes it hard to breathe. "Progressive" means the disease gets worse over time.

COPD can cause coughing that produces large amounts of mucus (a slimy substance), wheezing, shortness of breath, chest tightness, and other symptoms.

Cigarette smoking is the leading cause of COPD. Most people who have COPD smoke or used to smoke. Long-term exposure to other lung irritants, such as secondhand smoke, air pollution, chemical fumes, or dust, also may contribute to COPD. (Secondhand smoke is smoke in the air from other people smoking.)

In the United States, the term "COPD" includes two main conditions— emphysema and chronic bronchitis. Most people who have COPD have both conditions. Thus, the general term "COPD" is more accurate.

COPD is a major cause of disability, and it's the fourth leading cause of death in the United States.

COPD develops slowly. Symptoms often worsen over time and can limit your ability to do routine activities. Severe COPD may prevent you from doing even basic activities like walking, cooking, or taking care of yourself.

Your doctor will diagnose COPD based on your signs and symptoms, your medical and family histories, and test results.

COPD has no cure yet. However, treatments and lifestyle changes can help you feel better, stay more active, and slow the progress of the disease.

Quitting smoking is the most important step you can take to treat COPD. Other treatments include medicines, vaccines, pulmonary rehabilitation, oxygen therapy, and surgery. Your doctor also may recommend tips for managing complications.

You can take steps to prevent COPD before it starts. The best way to prevent COPD is to not start smoking or to quit smoking. Also, try to avoid other lung irritants that can contribute to COPD.

If you have COPD, you can take steps to manage your symptoms and slow the progress of the disease. Quit smoking and try to avoid other lung irritants. Also, get ongoing care, manage the disease and its symptoms, and prepare for emergencies.

If you have COPD, you may benefit from a clinical trial. Clinical trials test new ways to prevent, diagnose, or treat various diseases and conditions. For more information about clinical trials for COPD, talk with your doctor.